At Quanta Labs, we perform many IP tests for a variety of different industries. There are two standards for IP testing: IEC 60529 and ISO 20653. These standards aim to provide engineers with more detailed information than vague marketing terms such as waterproof or dustproof. This article provides an overview of exactly what IP ratings are and what level of protection for your product or application.
IP Testing Overview
IP (Ingress Protection) ratings are classified by categorical codes and measure of an enclosure/electronics ability to resist items entering it. The adoption of this classification system promotes uniformity in methods of describing the protection provided by the enclosure and in the tests to prove the various degrees of protection, they now provide engineers with a convenient, practical way to compare levels of sealing.
The IP code is composed of two numerals:
The first numeral refers to the protection against solid objects and is rated on a scale from 0 (no protection) to 6 (no ingress of dust).
The second numeral rates the enclosure’s protection against liquids and uses a scale from 0 (no protection) to 9 (high-pressure hot water from different angles).
Where a characteristic numeral is not required to be specified, it shall be replaced by the letter “X” (“XX” if both numerals are omitted.) Additional letters and /or supplementary letters may be omitted without replacement. Where more than one supplementary letter is used, the alphabetic sequence shall apply.
Below are the tables which specify what each “digit” in the IP level relates to for the IEC standard.
IEC IP Testing

The tests establishing compliance with any one of the lower degrees of protection
need not necessarily be carried out provided that these tests would obviously be met if
applied i.e. passing an IP3x test would cover the requirements for IP1x test. Best thing is to check what your customer requires products level of protection or check the environment the product will be going into and performing tests.
Solids ingress protection IP5x and IP6x are concerned with dust protection. IP5x allows some dust to enter, but not enough to affect equipment operation. IP6x is fully dust-tight and requires a vacuum line through the enclosure. The vacuum tests are performed for a period of between two and eight hours, depending on how much air volume is drawn through the cabinet. The duration of the non-vacuum IP5x is eight hours.

Examples Products with IP rating
Most outdoor industrial products are rated IP67/IP67 which is the highest level of dust protection and IPx5 is protection against power washing. IPx7 is protection of product being submerged in water 1m below the surface. If products are likely to be cleaned using pressurized jets, they should be rated at IPX5 or above. IP ratings for handheld electronic devices tend to focus on keeping both users and contents safe from inadvertent contact with mechanical or wired parts, but it’s common to see IP ratings for full protection from water ingress (IP65+) depending on their intended application. RFID Lock Electric Door Lock is rated IP65.The Outdoor Industrial 4G Router and Yealink W59R Rugged Wireless Expansion Handset are rated IP67.
Here is an another example showing the IP rating for common household items to give a frame of reference.

The IEC standard is broader than the ISO standard which outlines the protection of electrical equipment in road vehicles while the IEC tests are more general purpose.
ISO IP Testing

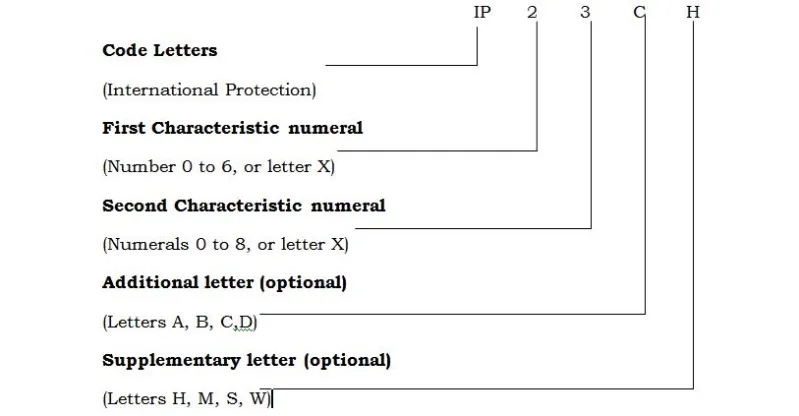
Here is an example of an IP test that can be quoted. IP16KB
The marking of an enclosure with the IP code IP16KB means:
(1) Protection of the electrical equipment within the enclosure against foreign objects with a
diameter of more than 50 mm (protection against foreign objects).
(6K) Protection of electrical equipment within the enclosure against harmful effects resulting
from water directed against the enclosure from any direction as a strong jet with increased
pressure (protection against water).
(B) Protection of persons against finger contact with hazardous parts within the enclosure \(protection against access).
The product would have to survive all three tests in order to be rated IP16KB. The standard doesn’t specific how many units need to pass in order for an enclosure to be rated. 1 unit is the minimum however testing more than one give the design and reliability engineering team more confidence.
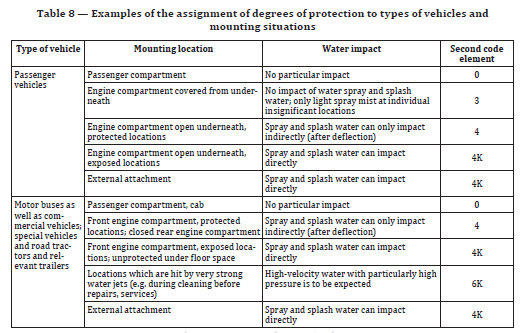
Unlike the IEC standard, the ISO standard offers the recommended IP test for the Type of vehicle and the mounting location of that vehicle.

Another notable difference between the ISO and IEC spec is the test IPx9k. IPx9 is testing from an IEC standard and is for electrical equipment while IPx9K is testing from an ISO standard and is for electrical equipment mounted on road vehicles. IPX9 testing requires that the force of a water jet is measured during the water test while IPX9K testing requires that the pressure of the water jet is measured during the water test.

- The distance for the test nozzle for the IPX9 test is 175 mm, plus or minus 25 mm and the ISO IPX9K test is 100 to 150 mm.
- The impact of the water is measured in terms of force for the IPX9 test while it is measured in terms of pressure for the IPX9K test.
Summary
At Quanta Labs, we perform many IP tests for a variety of different industries. There are two standards for IP testing: IEC 60529 and ISO 20653. These standards aim to provide engineers with more detailed information than vague marketing terms such as waterproof or dustproof. This article provides an overview of exactly what IP ratings are, how you can use them, and what level of protection for your product or application.
Some notable differences are:
- There are two standards for IP testing: IEC 60529 and ISO 20653. IP (Ingress Protection) rating are classified by categorical codes and measure of an enclosure/electronics ability to resist items entering it. The adoption of this classification system promotes uniformity in methods of describing the protection provided by the enclosure and in the tests to prove the various degrees of protection, they now provide engineers with a convenient, practical way to compare levels of sealing.
- The tests establishing compliance with any one of the lower degrees of protection
need not necessarily be carried out provided that these tests would obviously be met if
applied. - The standard doesn’t specific how many units need to pass in order for an enclosure to be rated. 1 unit is the minimum however different configurations can be tested.
- If products are likely to be cleaned using pressurized jets, they should be rated at IPX5 or above. IP ratings for handheld electronic devices tend to focus on keeping both users and contents safe from inadvertent contact with mechanical or wired parts, but it’s common to see IP ratings for full protection from water ingress (IP65+)
- IP5x allows some dust to enter, but not enough to affect equipment operation. IP6x is fully dust-tight and requires, a vacuum line through the enclosure.